|
|
Editorial
| ||||||
| The systemic implications of periodontitis: Dentist acquires a relevant role in general health | ||||||
| Alberto Rodríguez-Archilla1, Antonio Magán-Fernández2, Francisco Mesa3 | ||||||
|
1Associate Professor in Oral Medicine, University of Granada, Spain
2FPU Research Fellow, Clinical Medicine and Public Health PhD Program University of Granada, Spain 3Associate Professor in Periodontics, University of Granada, Spain | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Rodríguez-Archilla A, Magán-Fernández A, Mesa F. The systemic implications of periodontitis: Dentist acquires a relevant role in general health. J Case Rep Images Dent 2017;3:40–45. |
|
MICROBIOME: THE CONCEPT OF FOCAL INFECTION RE-EMERGES
| ||||||
|
The microbiota or human microbiome is the aggregate of microorganisms located in different places of the organism of healthy individuals. The microbiome participates in multiple physiological, metabolic, and immunological functions and its alteration, both quantitative and qualitative, can have significant consequences for general health [1]. The microbiome is very diverse and variable in and between individuals. The greatest diversity is located at the level of the gastrointestinal tract and mouth. Oral microbiota is the second most diverse of the organism, with more than 700 species of bacteria. Up to 350 different bacterial strains in marginal periodontitis and up to 150 strains in endodontic infection have been identified [2]. Under normal conditions, species of resident microorganisms in the oral cavity or other body surfaces are maintained in balance with the host in a dynamic biological interaction called symbiosis. When a disbalance in the oral microbiome occurs, appear the dysbiosis; allowing the bacteria to become pathogenic and cause diseases, such as caries and/or periodontal diseases, which could have a relevant impact on the general health [3]. The focal infection theory (FIT) states that these oral pathogens, their toxins or their metabolic sub-products may enter into the systemic circulation and move to distant parts, initiating a distant disease [4]. Oral bacteria play a role in various systemic conditions including cardiovascular disease, rheumatoid arthritis, adverse effects on pregnancy, osteoporosis, diabetes mellitus, stroke, inflammatory bowel disease and colorectal cancer, pancreatic cancer, respiratory tract infections, meningitis or brain abscess, abscesses in the lung, liver and spleen, appendicitis, pneumonia, obesity and Alzheimer’s disease [5][6] [7][8][9]. In various body regions such as atheromatous plaques, placenta and amniotic sac, respiratory tract, pancreas, joints or joint replacement implants, several periodontal pathogens (Porphyromonas gingivalis, Treponema denticola, Fusobacterium nucleatum or Campylobacter rectus) have been isolated [5]. Periodontitis is an infectious disease that affects the tooth-supporting tissues and exhibits a wide range of clinical, microbiological, and immunological manifestations. It is associated with and probably caused by a multifaceted dynamic interaction among specific infectious agents, host immune responses, hazardous environmental exposure, and genetic propensity [10]. Bacteria are essential to initiate the disease, but not sufficient to determine all cases of periodontitis. According to one US survey, chronic periodontitis affects around 35% of the adult population, with an even higher prevalence among the elderly [11]. According to WHO, this prevalence refers to a cohort of young adults aged between 35 and 44 years, an early onset periodontitis that appears before the age of 30 years, along with other connotations, known as aggressive periodontitis. Periodontal pathogens can enter the bloodstream and produce focal infections in different organs or systems. These distant lesions can be developed through three possible mechanisms [12][13]
| ||||||
|
PERIODONTAL MEDICINE – A MEDICAL RESEARCH LINE OF GREAT INTEREST
| ||||||
|
Kimmo Mattila et al. have commonly been credited with reigniting the interest in examining the relationship between oral and heart diseases in the latter half of the 1900s. In 1989, this group conducted a case-control study where they compared the oral health status, creating an oral index that included different periodontal parameters, of patients who had acute myocardial infarctions and healthy patients. The result, controlling classical cardiovascular risk factors, was a significant association between poor oral health and acute myocardial infarctions [14]. In 1994, Offenbacher was investigating delays in fetal growth in experimental models of periodontitis in hamster, publishing two years after, the first article that pointed to periodontitis as a possible risk factor for premature and/or low birth weight. In 1996, this author was the first to suggest the term Periodontal Medicine to refer to the systemic implications of periodontitis [15]. Taking as a starting point this work, research activity in periodontal medicine field has grown continuously, having been shown since then, up to 57 systemic pathologies related to periodontitis [16]. The dimension that is acquiring the systemic involvement of periodontitis, with questions that appear in scientific media, such as
Clearly implies the dentist in the general health of the patient in this new resurgence of the concept of focal infection. In this new paradigm, the dentist is responsible for the general well-being of the patient, although its field of action is the mouth. Periodontal lesion behaves as a potential source of chronic infection where bacteria, their products and/or inflammatory mediators go into the bloodstream and interact with distant target organs. Due to these consequences, the diagnosis and management of periodontitis should be considered as a public health problem [17]. | ||||||
|
SYSTEMIC DISEASES WITH MORE EVIDENCE RELATED TO PERIODONTITIS
| ||||||
|
According to the scientific evidence and the number of published articles, the systemic diseases most related to periodontitis are cardiovascular diseases, diabetes, adverse outcomes of pregnancy, rheumatoid arthritis, Alzheimer’s disease, and erectile dysfunction. | ||||||
|
PERIODONTITIS AND CARDIOVASCULAR DISEASES
| ||||||
|
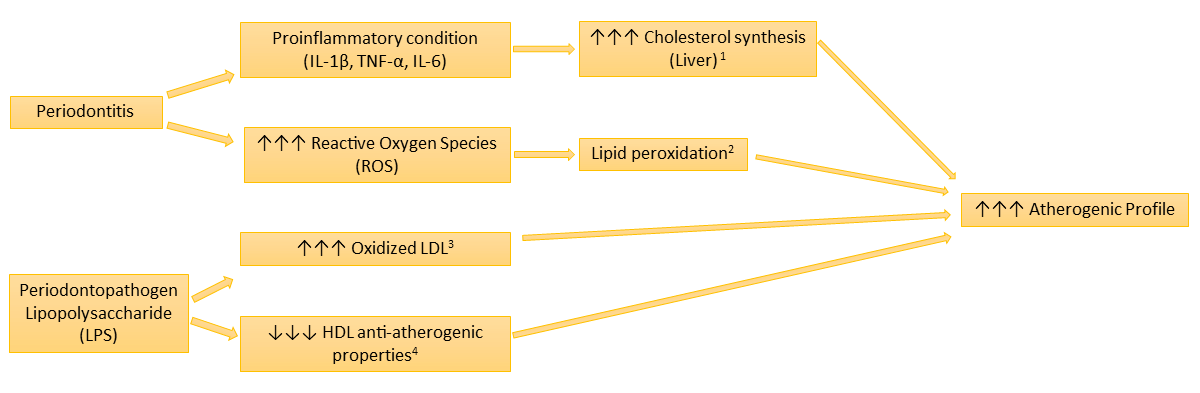
The PAROKRANK study, a recent large case-control study of periodontitis, verified by radiographic bone loss and with a careful consideration of potential confounders, concluded that the risk of a first myocardial infarction was significantly increased in patients with periodontitis even after adjustment for confounding factors (odds ratio, 1.28; 95% CI 1.03–1.60) [18]. Although there is a majority of observational studies that strengthen this association, not all of them support it. There is a fairly robust evidence that the pathogenic mechanism is due to an increased risk of endothelial dysfunction in patients with chronic periodontitis and subsequent development of atherosclerotic vascular disease [19]. In this sense, in chronic periodontitis, there is a clear increase in the atherogenic profile (Figure 1). To date, there are no intervention studies, based on periodontal treatment, that provide a clear evidence of a repercussion in cardio-cerebrovascular events. Further investigations with larger sample sizes and with longer follow-up periods are required to confirm a causal relation. Nevertheless, there is moderate evidence of improvement in indirect markers of cardiovascular disease, such as endothelial function and biomarkers of systemic inflammation, after periodontal treatment [20]. | ||||||
| ||||||
|
PERIODONTITIS AND DIABETES MELLITUS
| ||||||
|
Systemic proinflammatory cytokines associated with the periodontal inflammatory response such as C-reactive protein, IL-1ß, IL-6, TNF-a, increases resistance to insulin. TNF-a competes with insulin for cellular IRS-1 receptors, preventing permeability of membranes to glucose transit [21]. Periodontitis increases the functional failure of ß-cells pancreatic islets in mice with diabetes [22]. Patients with periodontal pockets = 6 mm, are 3.45 times more likely of developing diabetes [23], and periodontal disease was associated with five-year glycosylated hemoglobin A1c (HbA1c) progression in diabetes-free participants [24]. Periodontal treatment targeting the inflammation could decrease systemic proinflammatory cytokines and HbA1c levels. Several systematic reviews with meta-analyses on the effectiveness of periodontal treatment to improve glycemic control have been published. So far no overview of these systematic reviews has been performed. Faggion et al., analyzed eleven systematic reviews with meta-analyses where HbA1c was the most commonly used clinical endpoint. Meta-analytic estimates from systematic reviews generated an average reduction of 0.46% (median 0.40%) of HbA1c in patients with diabetes mellitus who received periodontal treatment. These meta-analyses had, nevertheless, methodological limitations such as inclusion of trials with different types of risk of bias that hinder more robust conclusions. Findings from this overview do not support the information that periodontal treatment may improve glycemic control [25]. A recent prospective cohort study with 120,000 patients treated at medical centers of the US Veterans Administration reported that periodontal treatment reduced HbA1c 0.02% at baseline and 0.07% at 1.7 years follow-up of periodontal maintenance [26]. | ||||||
|
PERIODONTITIS AND ADVERSE PREGNANCY OUTCOMES
| ||||||
|
Adverse pregnancy outcomes include births of low birth weight (<2500 g), very low birth weight (<1500 g), preterm birth (<37 weeks of gestation), very preterm birth (<32 weeks), growth restriction (weight for gestational age), preeclampsia, miscarriage, and stillbirth. Two hundred and seventy-one studies included in Web of Science (most of them cross-sectional, case-control, and cohort studies), 7 intervention studies with a sample size greater than 200 women and 12 systematic reviews and/or meta-analysis have attempted to demonstrate the relationship between periodontitis and preterm birth and/or low weight at birth. Most epidemiological association studies suggest that periodontitis may be a potential risk factor for preterm births, low birth weight or preeclampsia. Nevertheless, intervention studies, systematic reviews and/or meta-analysis, have not yet found sufficient scientific evidence of the influence of periodontal treatment on pregnancy [27]. The different demographic characteristics of the women, the types and severity of periodontitis, the different gestation periods of the participants, the variation in the composition of the microbiota and the different statistical methods used, seem to constitute confounding factors that preclude a firm conclusion from this topic. Periodontitis is an independent risk factor for adverse pregnancy outcomes [28]. Two probable biological mechanisms have been proposed to explain the relationship between periodontal infection and adverse pregnancy outcomes. The direct pathway, where a transient bacteremia in patients with periodontitis would cross the placental tissues triggering an inflammatory process that would induce birth. Recently, Blanc et al. determined in 57 biopsies of placentas (28 from mothers with periodontitis), 36 from preterm placentas and 21 from full-term placentas the presence of 15 oral bacteria using Nested-PCR. The placentas from women with periodontitis showed a higher prevalence of periodontal pathogens compared to those from women without periodontitis. Samples showed low prevalence of Actinomyces israelii, Parvimonas micra and Tannerella forsythia. The most ubiquitous bacterium, Fusobacterium nucleatum was more prevalent in mothers with periodontitis and preterm. These results show that oral bacteria may be normally present in the placenta, although, levels of certain oral pathogens in the placenta would highly depend on the mother’s periodontal state [29]. The indirect pathway where inflammatory cytokines locally produced in the gingival tissue would arrive through the bloodstream directly to the placenta or first to the liver where they would promote the production of other inflammatory cytokines and/or acute phase proteins, which finally would act, at the fetoplacental level, inducing birth [30]. IL-1ß, IL-6, TNF-a, and PGE2 appear to be the four major birth triggers cytokines, produced by TLR4 stimulation due to LPS of Gram-negative periodontal pathogens [31]. | ||||||
|
PERIODONTITIS AND RHEUMATOID ARTHRITIS
| ||||||
|
Rheumatoid arthritis is a chronic autoimmune inflammatory disease that affects synovial cavities, cartilage, and bones. Several infectious agents have been involved in the pathogenesis of this disease. Autoantibodies appear to be generated by molecular mimicry, especially between bacterial heat shock proteins and human Hsp60. The intestinal microbiome plays an important role in the etiology of this disease [5]. There is considerable evidence to support the interaction between periodontitis and rheumatoid arthritis. Periodontitis is up to eight times more severe in patients with rheumatoid arthritis compared to controls. Both diseases are characterized by inflammation and local destruction of soft and hard tissues. The pathogenesis of these diseases includes the release of cytokines and matrix metalloproteinases from inflammatory cells as well as osteoclast activator factors and RANK involvement. Susceptibility to rheumatoid arthritis and periodontitis could be related to some cytokines genes such as IL-1a + 4845, IL-1a-889, IL-1ß + 3954, IL-1ß -511 and TNF-a-308 [32]. In both rheumatoid arthritis and periodontitis, citrullination of peptides by activation of the enzyme peptidylarginine deiminase induces inflammation and cell death. In periodontitis patients, the overexpression of peptidylarginine deiminase, citrullinated proteins and anti-citrullinated peptide antibody (ACPA)-positive rheumatoid arthritis have been found. Moreover, infection with Porphyromonas gingivalis precedes the onset of rheumatoid arthritis and that antibodies against citrullinated protein titers (ACPA) are higher in aggressive periodontitis. On the other hand, patients with rheumatoid arthritis and periodontitis are more likely to be ACPA positive [33]. In both diseases are high levels of cytokines, matrix metalloproteinases, mediators derived from neutrophils and oxidative stress. Polymorphisms in the interleukin and Fc-γ receptor genes, as well as overexpression of the HLA-DRB1 allele, have been related to the etiopathogenesis of both diseases [34]. | ||||||
|
PERIODONTITIS AND ALZHEIMER’S DISEASE
| ||||||
|
Alzheimer’s disease is a chronic neurodegenerative disorder that leads to progressive and irreversible cognitive deterioration. Currently, this disease is the most common cause of dementia among older adults. The possible association between Alzheimer’s disease and periodontitis has been suggested in the biomedical literature. However, this association is still not well established. The infectious etiology of Alzheimer’s disease has been suggested and viral and/or bacterial infections may affect the neuronal axis through central nervous system (CNS) infection, comprising an episode of initiation or exacerbation of Alzheimer’s disease. Increases in serum levels of C-reactive protein and pro inflammatory and inflammatory cytokines such as tumor necrosis factor-alpha (TNFa) or interleukin 10 (IL 10) have been observed in both periodontitis and Alzheimer’s disease [35]. Some periodontal pathogens such as Porphyromonas gingivalis and Treponema denticola have been identified in the cerebrospinal fluid and neuronal ganglia. P. gingivalis has the ability to cross the blood-brain barrier and activate C3 complement fragment causing a neuronal lesion. Increased levels of antibodies against P. gingivalis have been related to higher rate of cognitive decline in Alzheimer’s disease [36]. | ||||||
|
PERIODONTITIS AND ERECTILE DYSFUNCTION
| ||||||
|
Penile erection is caused by the relaxation of the cavernous arteries and cavernous sinuses, with an increased blood flow to the penis, blood accumulation, and increased pressure in the cavernous bodies of the penis; these actions are mediated by the vasodilatory action of the combination nitric oxide— GMPc [37]. The two main sources of nitric oxide in the penis are adrenergic and non-cholinergic nerves, and the endothelium covering the arteries of the penis and cavernous sinuses [38] About 65% of the cases of erectile dysfunction are related to an organic cause, being the atherosclerotic cause the most common one [39]. An endothelial lesion due to an atheromatous plaque would be directly related to a decrease in nitric oxide levels. Vlachopoulos et al. found that the prevalence of erectile dysfunction was 47% in patients with cardiovascular disease and that severity (international erectile dysfunction index <10) and duration (> 24 months) indicated a more severe coronary involvement determined by angiography [40]. To date, only eleven articles have been published, all of them in the last six years, about the relationship between periodontitis and erectile dysfunction. Two of these articles were systematic reviews published in 2016. In a clinical trial, Eltas et al., pointed out that treatment of chronic periodontitis improved the degree of erectile dysfunction in Turkish population [41]. This association may be explained due to an endothelial dysfunction, provoked at the level of the vessels of the male sexual organs, either by the activation of proinflammatory cytokines from the oral focus of infection or by the direct action of the periodontopathogens. | ||||||
|
CONCLUSION
| ||||||
|
Increasingly, more evidence of the systemic repercussion of either oral pathogens or oral diseases is found. The practice of the dentist is not only conditions the survival of the teeth and the healing of oral mucosal lesions but also affects the overall general health of patients. The dentist must consider these associations; give a complete and often preventive medical advice about potentially life-threatening diseases that could be related to oral infections. The patients deserve it. Keywords: Focal infection, Infectious disease transmission, Vertical, Internal medicine, Periodontal diseases, Periodontal medicine | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Alberto Rodríguez-Archilla – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Antonio Magán-Fernández – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Francisco Mesa – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of Submission
The corresponding author is the guarantor of submission. |
|
Source of Support
None |
|
Conflict of Interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Alberto Rodríguez-Archilla et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|