|
|
Case Report
| ||||||
| Esthetic rehabilitation of poorly treated maxillary teeth: A one-year follow-up | ||||||
| Majd Abedrabbo1, Afaf Alnajajrah1 | ||||||
|
1BDS, Ebtisamati Dental Center, Arrass, Saudi Arabia.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Abedrabbo M, Alnajajrah A. Esthetic rehabilitation of poorly treated maxillary teeth: A one-year follow-up. J Case Rep Images Dent 2018;4:100025Z07MA2018. |
|
ABSTRACT
|
|
Introduction:
Full coverage ceramic restorations offer predictable treatment options in dentistry, but a certain amount of tooth structure must be removed to provide an adequate thickness of the ceramic material. Porcelain laminate veneers provide more conservative approach, utilizing the recent adhesive technologies with maximum bonding to the enamel surface.
Case Report: In this case, smile rehabilitation was planned in an interdisciplinary manner, in which selective esthetic crown lengthening, porcelain laminate veneers and lithium disilicate crowns were chosen. All available treatment modalities were discussed to reach the most durable and esthetic result. The treatment sequence was also discussed in details. Conclusion: Proper restoration design and execution are very critical keys for success; that should be confirmed by regular follow ups. Our patient was very satisfied with the result. Follow-up after one year shows the stable healthy appearance of the gingival tissues. | |
|
Keywords:
Crowns, Dental porcelain, Dental veneers, Smiling
| |
|
INTRODUCTION
| ||||||
|
Esthetic demand of patients increases day-by-day, enhancing our daily practice towards smile design and rehabilitation. Treatment modalities vary widely with the progressive development of dental materials, technologies and techniques. Smile design has become one of the widest multidisciplinary procedures in dentistry nowadays [1]. Healthy periodontium is one of the mandatory elements of a pleasant smile. Absence of inflammation, bleeding, swelling, pocketing and other signs of periodontal disease are crucial to obtain the desired esthetic result. However, the amount of gingival display, gingival architecture, clinical crown dimensions and tooth position play an important role in the esthetic value of the cosmetic restoration [2]. Therefore, an interdisciplinary approach is necessary to achieve the optimal result. Composite resins and ceramics are very popular in this field [3]. Each one has advantages and disadvantages that influence the choice of the used material. Composites are usually the first conservative approach with low cost, acceptable esthetics, minimal preparation needed and can be done chair side [3] [4]. On the other hand; polymerization shrinkage, marginal micro-leakage, plaque retention and shade instability are still big problems that face dentists [3]. Dental ceramics have become one of the promising tooth colored materials with superior optical properties that mimic natural teeth. Also, biocompatibility, wear resistance, high compressive strength and minimal plaque adherence have made ceramics an excellent choice [5]. However, some physical properties can be still a main concern that may affect the long term results. For example, brittleness, poor tensile strength and crack propagation may affect the long-term durability of the restoration. These weaknesses can be overcome by choosing the proper restoration design [3] [4],[5] [6]. The case report presented here describes the use of two different designs of ceramic restorations accompanied by gingival plastic surgery for maximal esthetic effect. | ||||||
|
CASE REPORT
| ||||||
|
A 31-year-old male presented to our clinic with multiple complaints regarding the smile. His main concern was to remove old white fillings that were done four years ago as a treatment of mild discoloration in the anterior teeth as he described. Full medical history was recorded, in which the patient is totally healthy. Clinical extraoral examination was done without any obvious abnormality. Temporomandibular joint (TMJ), regional lymph nodes, face symmetry and muscles of mastication were examined well. Intraoral clinical ( (Figure 1) and radiographic (periapical X-ray) (Figure 2) examination revealed a list of problems:
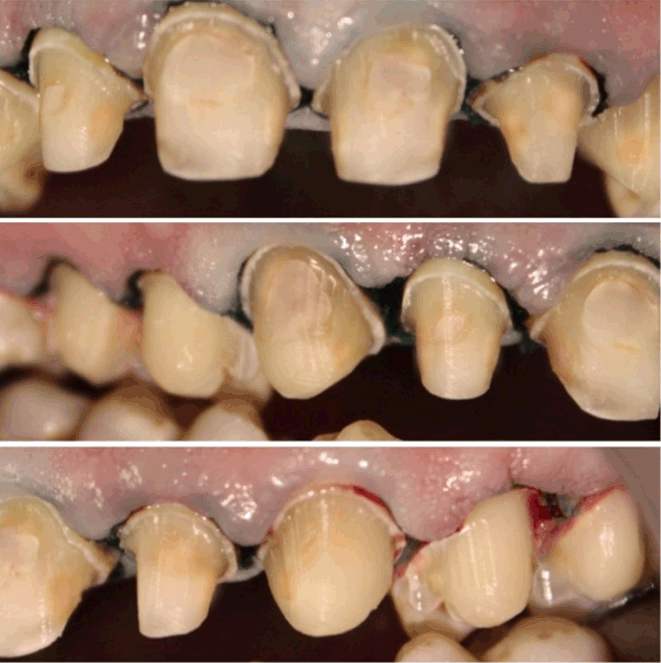
Treatment options were discussed with the patient. A decision was made to improve the esthetic appearance of all his upper teeth that show in the smile (including upper second premolars). First, selective crown lengthening would be done to level the gingival margins. Second, metal free crowns for upper anteriors, and veneers for upper premolars would be done. Improving oral hygieneScaling, polishing and oral hygiene instructions were given strictly. Smoothening of the poor over-hanged margins of the composite veneers was done. Chlorhexidine 0.2% mouthwash was prescribed twice daily after brushing and flossing. Appointment was given after one week for periodontal surgery. Crown lengtheningPeriodontal surgery was done for upper premolars and right lateral incisor. Conventional internal bevel incision was done using blade 15c, 2–3 mm away from the free gingival margin. Sulcular incision was done along the sulcus of the relevant teeth. Resected gingiva was removed by sickle scaler . Periodontal dressing was applied on the selected teeth. Postoperative instructions were given to the patient, with the advice to continue using chlorhexidine 0.2% mouthwash twice daily. A follow-up appointment was given after one week (Figure 3). Teeth preparation and impressionsAfter four weeks of surgery, the prosthetic part was started. Teeth were prepared using diamond burs to form an equigingival deep chamfer finish line for the crowns , and light chamfer for the veneers. A butt joint with partial buccal cusp coverage design was done for the premolars . Finishing discs were used to smooth and round the preparation angles (Figure 4). Moisture control was obtained by cotton rolls and saliva ejectors. Double retraction cords were used. Impressions were done using addition-cured silicon in metal trays, single stage technique (Figure 5). Shade was selected from Vitapan 3D Master shade guide. Provisional crowns were fabricated directly using acrylic resin and cemented temporarily. Consequently, bite registration at centric occlusion position using additional silicone and alginate impression for the lower arch were done. Disinfection for the impressions was done by immersion in sodium hypochlorite 1% for 10 minutes, and then sent to the ceramist. Metal free crowns were designed to achieve the desired esthetic goal. IPS e-max ZirCAD copings with IPS e-max Ceram layering were the choice for the crowns, IPS e-max lithium disilicate for the veneers . | ||||||
CementationThe patient was recalled. Provisional crowns were removed, try in was done using try in paste. The marginal integrity for each unit was checked individually. Occlusion in maximum intercuspation, lateral excursions, and protrusive movements was examined, in which a group function guidance was designed. No working and non- working interferences were found. The patient was completely satisfied with the shade and shape of the teeth. Therefore, a decision was taken to do permanent cementation. Moisture control and teeth isolation was well obtained. The whole prepared teeth were treated with 35% phosphoric acid etchant and single bond. The veneers were treated with 10% hydrofluoric acid etchant and silane coupling agent. Cementation was done with dual cured resin cement for the crowns, and light cured one for the veneers (Table 1). One week after cementation, the health of gingival tissues surrounding restorations were observed, enhancing the integration between ceramics, gingival margin and lips. The esthetic results were very satisfactory (Figure 6). The quality of the prosthesis and the appearance of the gingival margin were maintained after one-year follow-up (Figure 7 Figure 8).
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
DISCUSSION | ||||||
|
Treatment protocols for such a case were discussed deeply in many previous studies [7] [8] [9]. Composite veneers, porcelain laminate veneers and full ceramic crowns were suggested options. In one clinical study, there was no significant difference in patient satisfaction with composite or ceramic laminate veneers immediately after placement, but after two years of clinical service, patients were significantly more satisfied with the ceramic restorations [9]. In another study, survival rates for veneer restorations were 94% for porcelain restorations, 90% for indirect composite restorations and 74% for direct composite restorations [10]. Furthermore, direct resin composite veneers had a failure rate of 14% over three years of service, with a low incidence of marginal staining [9] [10]. Various clinical studies have shown that the survival rate for bonded porcelain laminate veneer restorations is more than 90% over 10 years of clinical service. In those studies, the failures reported were either cohesive ceramic fractures or failures of the adhesive between the cement and the tooth surface [11] [12] [13]. Adhesive-related failures could be attributed to the extent of tooth preparation. Particularly with deep preparations in dentin, less adhesion can be expected relative to enamel [10][11] [12] [13]. In fact, the bond strength of composite cement to enamel is in the range of 40 MPa, in which sometimes exceeds the cohesive strength of enamel itself [11]. Failure of the adhesive between cement and enamel was rarely observed. In addition to fractures, other types of failure, such as microleakage and debonding, have been reported [10] [11] [12] [13]. For full ceramic crowns, some studies reported a significant difference in the mean fracture resistance of veneered zirconia crowns and monolithic lithium disilicate crowns [14]. Zirconia cores are reported to be less translucent than glass, lithium disilicate, or alumina cores [15]. This can be beneficial to manufacture crowns that combine the strength of zirconia cores and the esthetics of the veneering glass. | ||||||
|
CONCLUSION | ||||||
|
This case report has described an interdisciplinary approach for obtaining the maximum esthetic result for maxillary teeth. Restoration design, clinical procedures and adhesion, which are considered key factors for clinical success, have been described. The rationale for various choices in this treatment protocol has been detailed with reference to the pertinent literature. | ||||||
|
REFERENCES
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Majd Abedrabbo – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Afaf Alnajajrah – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of Submission
The corresponding author is the guarantor of submission. |
|
Source of Support
None |
|
Consent Statement
Written informed consent was obtained from the patient for publication of this case report. |
|
Conflict of Interest
Authors declare no conflict of interest. |
|
Copyright
© 2018 Majd Abedrabbo et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|